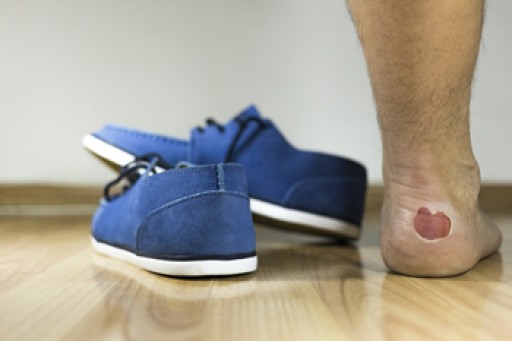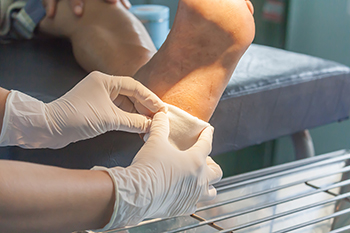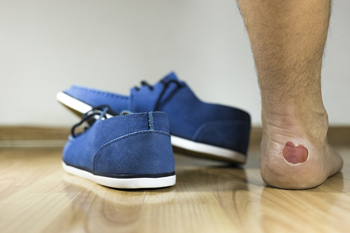
Blisters are fluid-filled pockets that typically form in the skin's upper layers after injury, commonly on feet. The fluid cushions the damaged area, aiding healing. Most blisters contain clear serum and heal naturally in three to seven days without medical intervention. Bursting them should be avoided to prevent infection or delays in healing. If they burst, allow drainage and cover with a sterile dressing. Blisters stem from various causes, including friction, heat, chemical contact, or medical conditions, like chickenpox. Preventing blisters involves wearing comfortable, well-fitting shoes, keeping feet dry with thicker socks or talcum powder, and applying sunscreen. If you have a foot blister that appears infected, is painful, or is recurring, it is suggested that you make an appointment with a podiatrist as soon as possible.
Blisters may appear as a single bubble or in a cluster. They can cause a lot of pain and may be filled with pus, blood, or watery serum. If your feet are hurting, contact one of our podiatrists of Canonsburg Podiatry Associates. Our doctors can provide the care you need to keep you pain-free and on your feet.
Foot Blisters
Foot blisters are often the result of friction. This happens due to the constant rubbing from shoes, which can lead to pain.
What Are Foot Blisters?
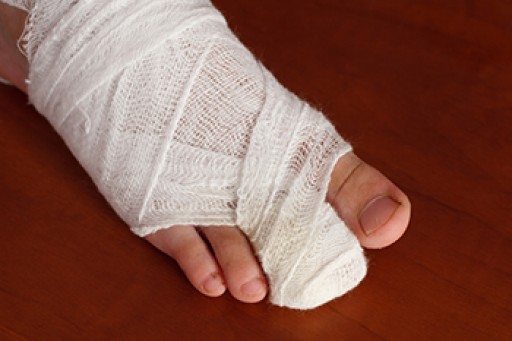
A foot blister is a small fluid-filled pocket that forms on the upper-most layer of the skin. Blisters are filled with clear fluid and can lead to blood drainage or pus if the area becomes infected.
Symptoms
(Blister symptoms may vary depending on what is causing them)
- Bubble of skin filled with fluid
- Redness
- Moderate to severe pain
- Itching
Prevention & Treatment
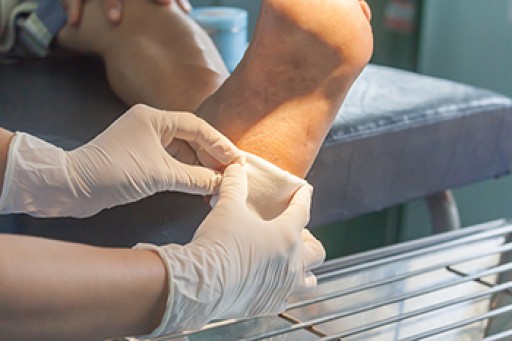
In order to prevent blisters, you should be sure to wear comfortable shoes with socks that cushion your feet and absorb sweat. Breaking a blister open may increase your chances of developing an infection. However, if your blister breaks, you should wash the area with soap and water immediately and then apply a bandage to the affected area. If your blisters cause severe pain it is important that you call your podiatrist right away.
If you have any questions, please feel free to contact our office located in Canonsburg and McMurray, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.